Microbiologically Documented Infection-related Mortality in Children with Acute Leukemia: A Single-center Experience
Microbiologically Documented Infections in Acute Leukemia
DOI:
https://doi.org/10.4274/jpea.2023.222Keywords:
Acute leukemia, febrile neutropenia, microbiologically documented infectionAbstract
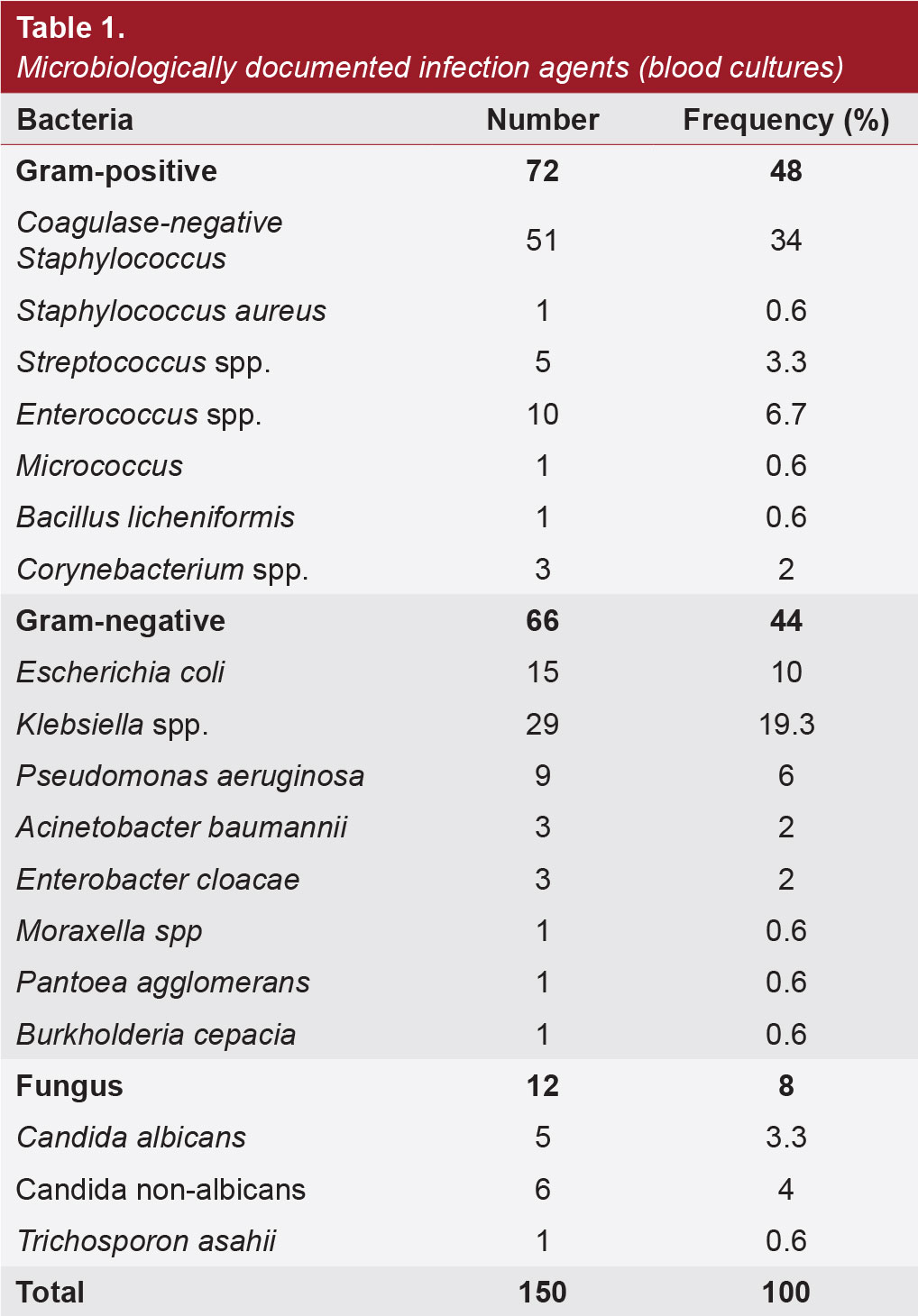
Infections are a significant cause of morbidity and mortality of chemotherapy-induced neutropenia in children with acute leukemia. The aim of this study was to evaluate microbiologically documented infections (MDIs) during febrile neutropenia (FN) episodes and their relation to mortality. Four hundred eighty-seven FN episodes of 140 children were enrolled in this single-center study, and MDI in those FN episodes was retrospectively examined. Eighty-four patients (60%) had at least one positive peripheral blood, central line, or urine culture. MDIs were detected in 163 of 487 (33.4%) FN episodes of 84 children with leukemia. Gram-negative bacteria, Gram-positive bacteria, and fungal agents were isolated in 52.7%, 40.4%, and 6.9% of whole episodes. Coagulase-negative Staphylococci and Enterococci were the most detected Gram-positive bacteria. Klebsiella spp. and Escherichia coli were the most common Gram-negative bacteria isolated in the entire cohort. A central line was present in 145 MDI episodes, and catheter removal was required in 35 cases (17.7%) due to infection with Gram-negative bacteria, Gram-positive bacteria 43%, 28.5%, and fungus 28.5%, respectively. MDI-related mortality was 9.8%. The highest mortality rate (16.7%) was observed in Gram-negative bacteria and patients with relapsed and resistant leukemia. The most common infectious agent related to mortality was Klebsiella (31%). Resistance to third- or fourth-generation cephalosporins in Gram-negative bacteria was found to be over 50% of our cohort uri. Empirical antibiotic therapy at the onset of FN in neutropenic patients is crucial; therefore, the institution’s predominant pathogens and resistance patterns should guide the choice of empirical antimicrobials. To reduce mortality and morbidity, each center should know its local epidemiological data and antibiotic susceptibility.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2023 The Journal of Pediatric Academy

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.








